Monday, 3 February 2025
How to Use Apple Cider Vinegar for Reducing Gum Sensitivity

Soothe Those Sensitive Gums with Apple Cider Vinegar: A Natural Approach
Hey there! Dealing with sensitive gums? That sharp, shooting pain when you bite into something cold or sweet? Ugh, I know the feeling. It's not fun, and it can really put a damper on enjoying your favorite foods. While a trip to the dentist is always a good idea if your sensitivity is persistent or severe, many people are exploring natural remedies to help manage their symptoms. One popular option gaining traction is apple cider vinegar (ACV). But does it actually work? And if so, how do you use it safely and effectively?
Let's dive into the world of ACV and gum sensitivity. This isn't medical advice – I'm just sharing information I've gathered and experiences I've heard from others. Always chat with your dentist before starting any new oral health routine, especially if you have existing dental issues.
Understanding Gum Sensitivity
Before we jump into ACV remedies, let's briefly touch on why our gums get sensitive in the first place. Sensitivity is often a sign that the protective enamel layer on your teeth is wearing away, exposing the dentin underneath. Dentin has tiny tubules that lead to the nerve in your tooth, making it vulnerable to temperature changes, sugary foods, and even pressure. Gum recession, where your gums pull back from your teeth, can also expose the roots, contributing to sensitivity.
Several things can cause gum recession and sensitivity:
- Aggressive brushing
- Gum disease (gingivitis or periodontitis)
- Grinding your teeth (bruxism)
- Certain medical conditions
- Poor oral hygiene
Addressing the underlying cause is crucial for long-term relief, but in the meantime, ACV might offer some temporary soothing effects.
How Apple Cider Vinegar Might Help Sensitive Gums
ACV's potential benefits for sensitive gums are primarily linked to its acidity and its antibacterial properties. The slightly acidic nature of ACV may help to neutralize the pH balance in your mouth, which can be disrupted by acidic foods and drinks. A balanced pH can potentially reduce the sensitivity by minimizing the exposure of the dentin tubules.
Furthermore, ACV contains acetic acid, which has shown some antibacterial properties in studies. While more research is needed specifically on its effect on gum health, this antibacterial action might help to control the bacteria associated with gum disease, a common contributor to sensitivity.
Important Note: The acidity of ACV is a double-edged sword. While it might offer some benefits, overuse can erode tooth enamel, leading to even more sensitivity and dental problems down the line. Always use it in moderation and follow the recommended methods carefully.
Using Apple Cider Vinegar for Gum Sensitivity: Safe and Effective Methods
There are a few ways you can incorporate ACV into your oral care routine. Remember, these are suggestions, and you should always consult your dentist before trying anything new.
The Rinse Method
This is arguably the most popular method. Mix a tablespoon of raw, unfiltered ACV (look for "with the mother") with a cup of water. Swish this solution gently around your mouth for about 30 seconds to a minute, ensuring it reaches all areas. Then, spit it out and rinse your mouth thoroughly with plain water. Do not swallow the mixture! Repeat this once or twice daily, but never more than that.
The Topical Application (Use with Caution!)
Some people dab a tiny amount of diluted ACV directly onto sensitive areas with a cotton swab. This method is significantly less recommended and needs extreme caution! The high acidity can damage your enamel more effectively than rinsing. If you choose this, dilute it heavily— perhaps a teaspoon of ACV to a tablespoon of water — and only do it sparingly.
Important Considerations and Precautions
While ACV is a natural remedy, it's crucial to be mindful of its potential drawbacks:
- Tooth Enamel Erosion: ACV's acidity can wear down your enamel over time if used excessively or incorrectly. Always dilute it properly and don't use it more often than recommended.
- Soreness and Irritation: Some people experience mild burning or discomfort when using ACV. If you notice this, immediately dilute it further or stop using it completely.
- Interactions with Medications: ACV can interact with certain medications. If you're taking any medications, consult your doctor or pharmacist before using it.
- Not a Replacement for Professional Care: ACV should be considered a complementary approach, not a replacement for regular dental checkups and professional dental hygiene. If your sensitivity persists or worsens, see your dentist immediately.
Alternatives and Complementary Approaches
Alongside ACV, consider these strategies to manage gum sensitivity:
- Gentle Brushing Technique: Use a soft-bristled toothbrush and brush gently, avoiding aggressive scrubbing.
- Fluoride Toothpaste: Fluoride helps strengthen enamel and can reduce sensitivity.
- Desensitizing Toothpaste: These toothpastes contain ingredients that block the tubules in your dentin, reducing sensitivity.
- Mouthguard for Bruxism: If you grind your teeth, a mouthguard can protect your teeth and gums.
- Healthy Diet: A balanced diet rich in vitamins and minerals supports overall oral health.
Commonly Asked Questions
Q: How long does it take to see results from using ACV for gum sensitivity?
A: Results vary from person to person. Some people might notice a difference within a few days, while others might not see significant improvement. Consistency is key, but if you don't see improvement after a week or two, stop using ACV and consult your dentist.
Q: Can I use ACV if I have gum disease?
A: While ACV has some antibacterial properties, it's not a treatment for gum disease. If you have gum disease, you need professional dental care. ACV might provide temporary relief from some symptoms, but it won't address the underlying infection.
Q: What type of apple cider vinegar should I use?
A: Use raw, unfiltered apple cider vinegar, often labeled as "with the mother." This type contains more beneficial components.
Q: Can I swallow the ACV rinse?
A: No! ACV is acidic and swallowing it can upset your stomach. Always rinse thoroughly with plain water after using the ACV rinse.
Q: Is it okay to use ACV every day?
A: No, it's best to limit your ACV rinse to once or twice a day, at most. Overuse can damage your enamel.
Remember, this information is for general knowledge and shouldn't replace professional dental advice. If you're concerned about your gum sensitivity, please schedule an appointment with your dentist for a proper diagnosis and treatment plan.
Treating Gum Recession with Probiotics: A Natural Approach

Treating Gum Recession with Probiotics: A Natural Approach
Gum recession, the process where gum tissue pulls back from the teeth, exposing the tooth roots, is a prevalent dental concern affecting millions worldwide. While traditional treatments exist, ranging from surgical procedures to scaling and root planing, there's a growing interest in exploring natural and complementary approaches to manage and potentially reverse gum recession. Probiotics, live microorganisms that confer health benefits when administered, have emerged as a potential candidate in this field, although further research is necessary to confirm their efficacy definitively.
Understanding Gum Recession and its Etiology
Gum recession, clinically termed gingival recession, is a gradual process that can lead to significant oral health complications. The exposed tooth roots become vulnerable to sensitivity, decay, and even tooth loss. Several factors contribute to gum recession, including:
- Aggressive brushing: Vigorous brushing with a hard-bristled toothbrush can abrade the gum tissue over time, causing recession.
- Periodontal disease: Gingivitis and periodontitis, inflammatory diseases affecting the gums and supporting structures of the teeth, are major contributors to gum recession. Bacterial infection and the body's inflammatory response lead to tissue breakdown and bone loss.
- Genetics: A genetic predisposition can increase the susceptibility to gum recession, with some individuals naturally having thinner or more fragile gum tissue.
- Bruxism: Teeth grinding or clenching puts excessive pressure on the teeth and gums, potentially leading to recession.
- Hormonal changes: Fluctuations in hormone levels, particularly during pregnancy or menopause, can affect gum health and increase the risk of recession.
- Smoking: Smoking impairs the body's ability to heal and fight infection, exacerbating periodontal disease and contributing to gum recession.
- Misaligned teeth: Malocclusion, or improperly aligned teeth, can place uneven pressure on the gums, leading to recession in certain areas.
The Role of the Oral Microbiome in Gum Health
The oral cavity houses a complex ecosystem of microorganisms, collectively known as the oral microbiome. A balanced microbiome is crucial for maintaining oral health. An imbalance, known as dysbiosis, characterized by an overgrowth of harmful bacteria and a reduction in beneficial bacteria, is strongly linked to the development and progression of periodontal disease, a major cause of gum recession.
Harmful bacteria produce toxins that inflame the gums, leading to tissue destruction and bone loss. Conversely, beneficial bacteria can help maintain a healthy balance within the oral microbiome, preventing the proliferation of harmful pathogens. This is where probiotics come into play.
Probiotics and their Potential in Treating Gum Recession
Probiotics, primarily lactic acid bacteria (LAB) and bifidobacteria, are known for their ability to modulate the gut microbiome and improve gut health. Research suggests that their beneficial effects may extend to the oral cavity as well. Several mechanisms are proposed through which probiotics could help address gum recession:
- Inhibition of pathogenic bacteria: Probiotics can compete with harmful bacteria for nutrients and attachment sites, limiting their growth and reducing their ability to cause inflammation.
- Production of antimicrobial substances: Some probiotic strains produce substances like bacteriocins, which directly inhibit the growth of harmful bacteria.
- Modulation of the immune response: Probiotics can influence the immune system by reducing inflammation and promoting tissue repair. They may stimulate the production of antibodies and other immune factors that combat periodontal pathogens.
- Enhancement of tissue regeneration: Some studies suggest that probiotics may stimulate the production of growth factors that promote tissue regeneration and repair, potentially aiding in the regeneration of gum tissue.
Specific Probiotic Strains Showing Promise
While research is still ongoing, several probiotic strains have shown promise in preclinical and clinical studies for improving oral health. These include Lactobacillus reuteri, Lactobacillus salivarius, Lactobacillus rhamnosus, and Streptococcus salivarius. However, it's crucial to note that the results are not universally consistent, and more research is required to establish definitive clinical efficacy.
Challenges and Limitations of Probiotic Therapy for Gum Recession
Despite the potential benefits, several challenges and limitations exist in using probiotics to treat gum recession:
- Limited clinical evidence: While preclinical studies have shown promising results, large-scale, well-designed clinical trials are needed to confirm the efficacy and safety of probiotics in treating gum recession.
- Strain specificity: The effects of probiotics are strain-specific. Not all probiotic strains are equally effective in improving oral health, and identifying the most effective strains for gum recession requires further research.
- Delivery methods: Effective delivery of probiotics to the oral cavity can be challenging. Simply rinsing with a probiotic solution may not be sufficient to achieve therapeutic concentrations at the site of infection.
- Individual variability: The response to probiotic therapy can vary considerably among individuals, depending on factors like the composition of their oral microbiome, overall health status, and other lifestyle factors.
- Potential side effects: Although generally considered safe, some individuals may experience mild side effects such as digestive upset or allergic reactions.
Conclusion and Future Directions
Probiotics offer a potentially promising natural approach to manage gum recession by modulating the oral microbiome and reducing inflammation. However, the current evidence is insufficient to recommend probiotics as a standalone treatment for gum recession. More rigorous clinical trials are necessary to confirm their efficacy and establish optimal delivery methods and dosages. In the meantime, maintaining excellent oral hygiene, including regular brushing, flossing, and professional dental cleanings, remains crucial in preventing and managing gum recession. Probiotics may serve as a valuable complementary therapy, but they should not replace conventional dental care.
Future research should focus on identifying the most effective probiotic strains for treating gum recession, developing effective delivery systems, and conducting large-scale clinical trials to establish the efficacy and safety of probiotic therapy. Furthermore, studies exploring the combination of probiotics with other natural therapies or conventional treatments could provide even more effective strategies for managing gum recession and improving overall oral health.
How to Treat Bleeding Gums from Gum Disease Naturally
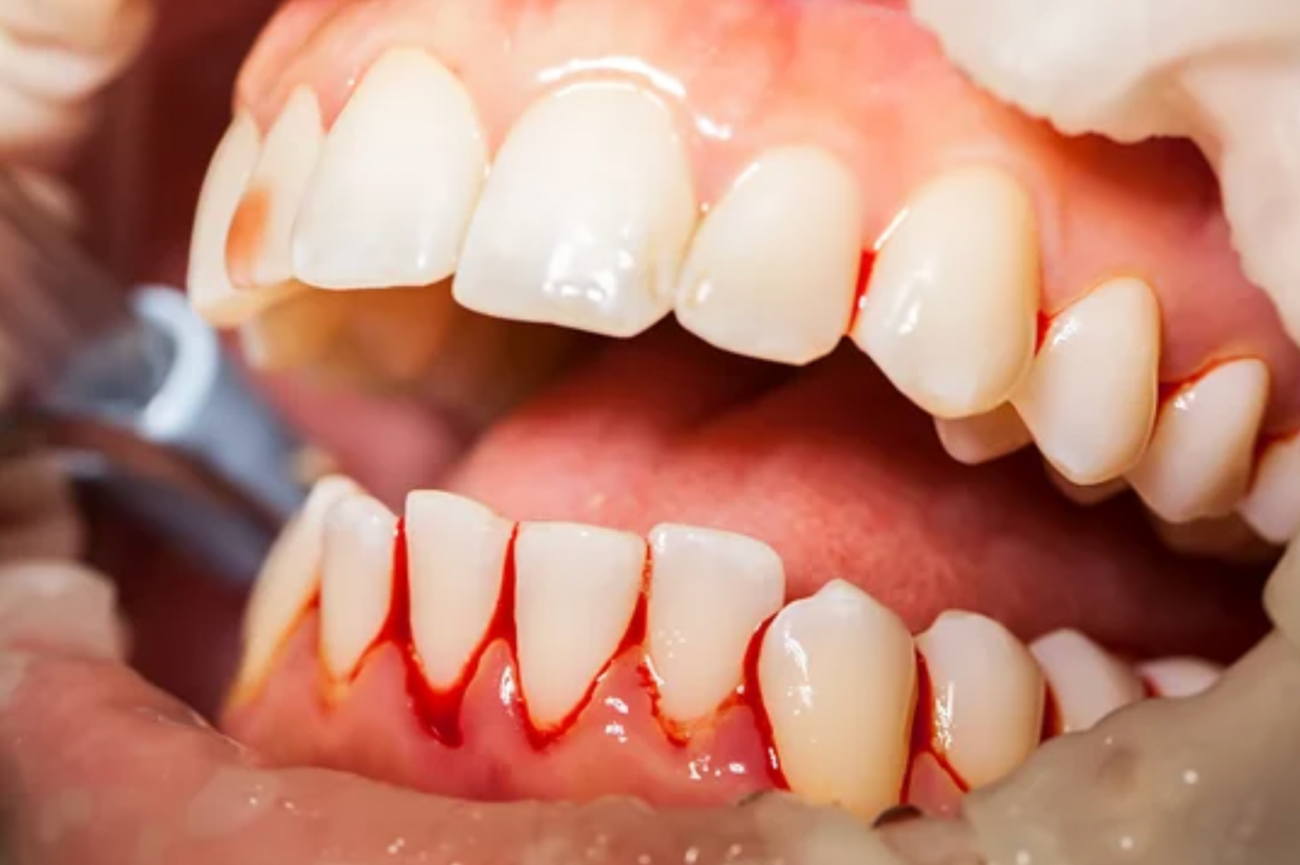
Naturally Treating Bleeding Gums from Gum Disease
Hey there! So, you've got bleeding gums, and you're worried it might be gum disease. That's understandable – nobody wants to deal with that! Before we dive in, let me be clear: **I'm not a doctor, and this isn't a replacement for professional dental advice.** If you're experiencing bleeding gums, especially if it's persistent or accompanied by other symptoms like pain, swelling, or loose teeth, **you absolutely need to see a dentist ASAP.** This article is just to give you some information on natural approaches that *might* help support your treatment *in conjunction with* professional care, not replace it.Understanding the Root of the Problem: Gum Disease
Gum disease, or periodontal disease, is a serious infection that damages the soft tissues and bones that support your teeth. It starts with gingivitis, a mild form of gum inflammation, often characterized by red, swollen, and bleeding gums. If left untreated, gingivitis can progress to periodontitis, a more severe stage where the gums pull away from the teeth, forming pockets that harbor bacteria. These pockets can become infected, leading to bone loss and potentially tooth loss.Natural Approaches to Help Manage Bleeding Gums
Now, let's talk about some natural approaches that might help ease bleeding gums and support overall gum health. Remember, these are supportive measures, not cures.1. Improving Your Oral Hygiene Routine: The Foundation
This might seem obvious, but it's the absolute cornerstone of gum health. Are you *really* brushing and flossing properly? I'm talking twice a day, for at least two minutes each time, with gentle but thorough brushing, and using the right technique to floss effectively.Here's what to focus on:
- Brush gently: Aggressive brushing can damage your gums. Use a soft-bristled toothbrush and make small, circular motions.
- Floss daily: Flossing removes plaque and food particles from between your teeth, where your toothbrush can't reach.
- Use an antimicrobial mouthwash (with your dentist's okay): Some mouthwashes contain ingredients that can help reduce bacteria in your mouth.
- Consider an electric toothbrush: Many find electric toothbrushes make it easier to maintain a consistent and effective brushing technique.
2. The Power of Herbs and Essential Oils
Several herbs and essential oils possess antibacterial and anti-inflammatory properties that may help reduce gum inflammation and bleeding. Always dilute essential oils before using them in your mouth! Never apply undiluted essential oils directly to your gums.- Tea Tree Oil: Known for its antimicrobial properties. Dilute a few drops in a carrier oil like coconut oil and gently massage it onto your gums. (Again, consult your dentist before using this or any other essential oil).
- Myrrh: This ancient herb has been traditionally used for its healing properties. You can find myrrh extract in some mouthwashes or gums.
- Aloe Vera: Its soothing and anti-inflammatory properties may help calm irritated gums. You can apply aloe vera gel directly to your gums.
3. Dietary Changes for a Healthier Mouth
What you eat significantly impacts your oral health. A diet rich in fruits, vegetables, and whole grains provides essential nutrients that support gum health.- Vitamin C: Crucial for collagen production, which is essential for healthy gums. Citrus fruits, berries, and peppers are good sources.
- Vitamin K: Important for blood clotting, which can help reduce bleeding. Leafy green vegetables are excellent sources.
- Calcium: Essential for strong bones and teeth. Dairy products, leafy greens, and fortified foods are good sources.
- Reduce sugary foods and drinks: Sugar feeds the bacteria that cause gum disease.
4. Staying Hydrated: It's More Important Than You Think
Drinking plenty of water helps wash away food particles and bacteria from your mouth, keeping your gums cleaner and healthier.5. Stress Management: Believe it or Not, It Matters
Chronic stress can weaken your immune system, making you more susceptible to infections, including gum disease. Finding healthy ways to manage stress, like exercise, meditation, or yoga, can benefit your overall health, including your oral health.Important Considerations
* **Consistency is key:** These natural remedies won't work overnight. You need to be consistent with your oral hygiene and any natural treatments you choose. * **Listen to your body:** If your bleeding gums worsen or you experience new symptoms, seek professional dental care immediately. * **Don't delay professional care:** Natural remedies can be supportive, but they are not a substitute for regular dental checkups and professional treatment of gum disease.Commonly Asked Questions
Q: Will these natural remedies cure my gum disease?
A: No, these remedies are supportive measures to help manage symptoms and promote overall gum health. They cannot cure gum disease, which requires professional dental intervention.
Q: How long will it take to see results?
A: It varies depending on the severity of your gum disease and your commitment to oral hygiene and treatment. You might notice some improvement in bleeding within a few weeks, but significant changes may take longer.
Q: Can I use these remedies if I'm pregnant or breastfeeding?
A: Always consult your doctor or dentist before starting any new treatment, especially if you're pregnant or breastfeeding. Some herbs and essential oils may not be safe during these periods.
Q: What should I do if my gums are still bleeding after trying these remedies?
A: If bleeding persists or worsens, schedule an appointment with your dentist immediately. This is crucial to rule out more serious issues and get appropriate treatment.
Remember, taking care of your gums is an ongoing process. By combining good oral hygiene with a healthy lifestyle and seeking professional dental care when needed, you can significantly improve your gum health and keep that smile bright!Sunday, 2 February 2025
The Power of Probiotics for Supporting Healthy Gums Naturally

The Power of Probiotics for Supporting Healthy Gums Naturally
Maintaining optimal oral health is crucial for overall well-being. While traditional dental hygiene practices remain paramount, emerging research highlights the significant role of probiotics in supporting healthy gums and preventing periodontal diseases. This article explores the complex relationship between oral microbiota, probiotics, and gum health, delving into the mechanisms of action, supporting evidence, and potential future applications of probiotic therapies in periodontal care.
Understanding the Oral Microbiome and its Impact on Gum Health
The human mouth harbors a diverse and complex ecosystem of microorganisms, collectively known as the oral microbiome. This intricate community comprises bacteria, archaea, fungi, and viruses, interacting dynamically with the host's immune system and oral tissues. A balanced oral microbiome is essential for maintaining oral health. However, dysbiosis—an imbalance in the microbial community—can lead to the development of various oral diseases, most notably gingivitis and periodontitis.
The Role of Dysbiosis in Periodontal Disease
Periodontitis, a chronic inflammatory disease affecting the tissues supporting the teeth, is characterized by the destruction of periodontal ligaments and alveolar bone. This destructive process is primarily driven by dysbiosis, where pathogenic bacteria proliferate, overwhelming the beneficial commensal bacteria. Key periodontal pathogens, such as Porphyromonas gingivalis, Aggregatibacter actinomycetemcomitans, and Tannerella forsythia, produce potent virulence factors that contribute to inflammation, tissue breakdown, and bone loss.
The Protective Role of Commensal Bacteria
Conversely, a healthy oral microbiome is characterized by a predominance of commensal bacteria, which contribute to maintaining homeostasis and protecting against pathogenic invasion. These beneficial bacteria compete with pathogens for nutrients and attachment sites, produce antimicrobial substances, and modulate the host's immune response. A balanced microbiome, therefore, is crucial for preventing the onset and progression of periodontal diseases.
Probiotics: A Natural Approach to Restoring Oral Microbial Balance
Probiotics, defined as live microorganisms that confer a health benefit on the host when administered in adequate amounts, are increasingly recognized for their potential therapeutic applications in various areas of medicine, including dentistry. Oral probiotics aim to restore or maintain a healthy oral microbiome by either directly inhibiting pathogenic bacteria or indirectly enhancing the host's immune defenses.
Mechanisms of Action of Oral Probiotics
The beneficial effects of oral probiotics on gum health are mediated through several mechanisms:
- Competitive Exclusion: Probiotics compete with pathogenic bacteria for nutrients and binding sites on the tooth surface and gingival epithelium, thereby preventing their colonization and growth.
- Antimicrobial Substance Production: Certain probiotic strains produce bacteriocins and other antimicrobial compounds that directly inhibit the growth of periodontal pathogens.
- Immune Modulation: Probiotics can modulate the host's immune response by enhancing the production of antimicrobial peptides, increasing the activity of immune cells, and reducing inflammation.
- Improved Host Defense Mechanisms: By strengthening the host's defenses against infection and inflammation, probiotics contribute indirectly to maintaining a healthy oral environment.
Scientific Evidence Supporting the Use of Probiotics in Gum Health
While research on the efficacy of oral probiotics is still ongoing, a growing body of evidence suggests their potential benefits in supporting healthy gums. Several studies have demonstrated that specific probiotic strains, such as Lactobacillus species and Streptococcus salivarius, can reduce gingival inflammation, improve periodontal parameters, and decrease the levels of periodontal pathogens.
Clinical Trials and Observational Studies
Numerous clinical trials and observational studies have investigated the effects of probiotic interventions on periodontal health. These studies have generally shown promising results, with many reporting significant reductions in gingival bleeding, plaque index, and probing depth after probiotic administration. However, the results have varied across studies, likely due to differences in probiotic strains, dosage, delivery methods, and study designs.
Challenges and Limitations of Current Research
Despite the promising findings, several challenges and limitations need to be addressed in future research. These include:
- Standardization of probiotic strains and formulations: The lack of standardization in probiotic strains and formulations makes it difficult to compare the results of different studies.
- Optimal dosage and duration of treatment: The optimal dosage and duration of probiotic treatment for periodontal disease are yet to be determined.
- Delivery methods: Effective delivery methods are crucial for ensuring that probiotics reach the target site in sufficient numbers.
- Long-term efficacy and safety: Long-term studies are needed to assess the long-term efficacy and safety of probiotic interventions.
Future Directions and Potential Applications
The field of probiotic dentistry holds immense potential for developing innovative approaches to prevent and treat periodontal diseases. Future research should focus on identifying the most effective probiotic strains, optimizing delivery methods, and establishing clear clinical guidelines for the use of probiotics in periodontal care.
Personalized Probiotic Therapies
Advances in genomics and microbiome profiling may enable the development of personalized probiotic therapies tailored to the individual's unique oral microbiome composition. This approach could optimize treatment efficacy and minimize the risk of adverse effects.
Combination Therapies
Combining probiotics with other therapeutic modalities, such as scaling and root planing, may enhance treatment outcomes and improve periodontal health. Further research is warranted to explore the synergistic effects of probiotic therapies with conventional periodontal treatments.
Probiotic Mouthwashes and Toothpastes
The incorporation of probiotics into commercially available oral hygiene products, such as mouthwashes and toothpastes, could provide a convenient and accessible way to promote oral health and prevent periodontal disease. However, careful consideration must be given to ensure the viability and stability of probiotics in these products.
In conclusion, probiotics show promising potential as a natural and effective approach to supporting healthy gums. While further research is needed to fully elucidate their mechanisms of action and optimize their therapeutic applications, the accumulating evidence suggests that probiotics could play a significant role in the future of periodontal care, offering a valuable adjunct to conventional treatments and paving the way for personalized strategies to maintain optimal oral health.
How Cranberries Support Gum Health and Prevent Tooth Decay

Cranberries and Oral Health: A Comprehensive Review of their Potential Benefits
The relationship between diet and oral health is well-established. While diligent brushing and flossing remain cornerstones of preventative dentistry, emerging research highlights the potential contributions of certain dietary components to oral hygiene. Among these, cranberries have garnered significant attention due to their unique phytochemical profile and demonstrated antimicrobial properties. This review comprehensively explores the mechanisms by which cranberries may support gum health and prevent tooth decay, emphasizing the current scientific understanding and highlighting areas requiring further investigation.
The Phytochemical Composition of Cranberries and their Relevance to Oral Health
Cranberries (Vaccinium macrocarpon) are rich in a variety of bioactive compounds, many of which contribute to their purported health benefits, including those related to oral health. These compounds primarily include:
Proanthocyanidins (PACs): The Key Players
Proanthocyanidins (PACs), a type of condensed tannins, are considered the primary bioactive compounds responsible for the purported oral health benefits of cranberries. These polyphenols are potent antioxidants with demonstrable antimicrobial properties. Specifically, cranberry PACs have been shown to inhibit the adhesion of oral bacteria, particularly Streptococcus mutans, a key causative agent of dental caries (tooth decay).
The mechanism of action involves the unique structure of A-type PACs found in cranberries. These PACs possess a higher degree of polymerization and a unique configuration that allows them to effectively bind to the surface proteins of S. mutans, preventing their adherence to tooth enamel. This inhibition of bacterial adhesion is crucial, as it disrupts the formation of dental plaque biofilm, a sticky matrix of bacteria that promotes tooth decay and gum disease.
Other Beneficial Compounds
Beyond PACs, cranberries contain other phytochemicals that may contribute to their oral health benefits. These include:
- Organic acids: Cranberries contain significant amounts of organic acids, such as benzoic acid, malic acid, and quinic acid. These acids contribute to a low pH environment in the mouth, which may inhibit bacterial growth.
- Flavonoids: Cranberries are a source of various flavonoids, which possess antioxidant and anti-inflammatory properties. These properties may help to combat oxidative stress and inflammation associated with periodontal disease.
- Vitamins and Minerals: While not as prominent as the polyphenols, cranberries provide modest amounts of vitamins and minerals, some of which play a role in maintaining healthy gums and teeth. For example, Vitamin C is essential for collagen synthesis, crucial for gum tissue health.
Cranberries and the Prevention of Tooth Decay
The primary mechanism by which cranberries may prevent tooth decay lies in their ability to inhibit the adherence of S. mutans. As mentioned, the A-type PACs in cranberries effectively block the bacterial adhesion, thereby reducing the formation of dental plaque. A lower plaque buildup translates to a decreased likelihood of acid production by bacteria, which is the primary cause of enamel demineralization and subsequent tooth decay.
Numerous in vitro studies have demonstrated the effectiveness of cranberry extracts in inhibiting S. mutans adhesion. However, the translation of these findings to in vivo (human) studies has been less consistent. While some human studies have shown promising results, others have yielded less definitive outcomes, possibly due to variations in cranberry product formulations, dosage, and study methodologies. Further well-designed clinical trials are warranted to confirm the efficacy of cranberry consumption in preventing tooth decay in humans.
Cranberries and the Support of Gum Health (Periodontal Health)
Periodontal disease, encompassing gingivitis and periodontitis, is a chronic inflammatory condition affecting the gums and supporting structures of the teeth. The etiology of periodontal disease is complex, involving a dysbiotic microbial community within the periodontal pocket and a dysregulated host immune response. Cranberries may exert beneficial effects on periodontal health through several mechanisms:
Anti-inflammatory Effects
The flavonoids and other antioxidants present in cranberries may contribute to their anti-inflammatory effects. By reducing oxidative stress and modulating inflammatory pathways, cranberries could potentially help mitigate the inflammation associated with periodontal disease. However, direct evidence supporting this assertion in humans is still limited and needs further investigation.
Antimicrobial Effects against Periodontal Pathogens
While the anti-adhesion effects of cranberry PACs are most prominent against S. mutans, some studies suggest that cranberry extracts may also exhibit antimicrobial activity against other periodontal pathogens. This effect could contribute to a reduction in the bacterial load within the periodontal pocket, thus reducing inflammation and supporting gum health. However, more research is needed to determine the extent of this antimicrobial effect against a broader range of periodontal bacteria.
Challenges and Future Directions
Despite the promising preclinical and some clinical data, there are challenges in definitively establishing the oral health benefits of cranberries. These challenges include:
- Variability in Cranberry Products: The concentration of bioactive compounds, particularly PACs, can vary significantly across different cranberry products (juices, extracts, supplements). This variability makes it difficult to standardize the dosage and efficacy of cranberry interventions in clinical trials.
- Limited Clinical Evidence: While in vitro studies are supportive, more well-designed, large-scale, randomized controlled trials in humans are necessary to confirm the clinical efficacy of cranberries in preventing tooth decay and promoting periodontal health.
- Complex Interactions: The oral microbiome is incredibly complex, and the interaction of cranberry compounds with this diverse microbial community is not fully understood. Further research is required to elucidate these intricate interactions.
Future research should focus on standardizing cranberry products, conducting robust clinical trials with well-defined outcome measures, and investigating the complex interactions between cranberry components and the oral microbiome. This research will provide a stronger evidence base to support the potential role of cranberries in enhancing oral hygiene and preventing oral diseases.
In conclusion, while cranberries show promise as a complementary approach to traditional oral hygiene practices, more comprehensive research is needed to fully delineate their effectiveness in promoting gum health and preventing tooth decay. Currently available evidence points to the potential benefits of cranberry consumption, particularly its impact on reducing S. mutans adhesion, but further investigation is essential to translate this potential into robust clinical recommendations.
How to Treat Gum Infection from Brushing Too Hard with Natural Remedies

So You Brushed Too Hard...Now You've Got Gum Trouble? Let's Fix It Naturally!
Okay, we've all been there. You're aiming for that squeaky-clean feeling, and suddenly, you realize you've been a little *too* enthusiastic with the toothbrush. Ouch! That stinging, tender feeling in your gums? That's likely the start of a gum infection, possibly gingivitis, brought on by your overzealous brushing. Don't worry, though – before you panic and run to the dentist (which you *should* do if things get really bad!), let's explore some natural remedies that can help soothe those irritated gums and get you back on track to a healthy smile.
It's important to remember that while these natural remedies can be incredibly helpful for managing mild gum infections, they aren't a replacement for professional dental care. If your gums are severely inflamed, bleeding profusely, or you have persistent pain, see your dentist immediately. This is especially crucial if you notice any signs of infection like pus or significant swelling.
Understanding the Problem: Why Brushing Too Hard Hurts
Aggressive brushing, even with a soft-bristled toothbrush, can damage your gum tissue. Think of your gums as delicate skin – scrubbing too hard will irritate and inflame them, creating the perfect breeding ground for bacteria. This inflammation leads to gingivitis, the earliest stage of gum disease. Symptoms can include red, swollen gums, bleeding during brushing, and sometimes bad breath.
The Importance of Gentle Brushing
The key to preventing gum problems is gentle, effective brushing. You don't need to scrub hard to remove plaque; rather, focus on small, circular motions, ensuring you reach every surface of your teeth. Consider using a toothbrush with extra-soft bristles and investing in a good electric toothbrush with a gentle setting. Many electric toothbrushes have pressure sensors that alert you if you're brushing too hard. A gentle touch is far more effective in the long run!
Natural Remedies for Gum Infection
Now, let's dive into some natural ways to help soothe those irritated gums and combat the infection. Remember, consistency is key – these remedies work best when used regularly.
Saltwater Rinse
This is a classic remedy for a reason! Saltwater has amazing antiseptic properties. Dissolve half a teaspoon of salt in a cup of warm water and swish it around your mouth for about 30 seconds, then spit it out. Do this several times a day. The salt helps draw out inflammation and can kill some of the bacteria contributing to the infection.
Aloe Vera
Aloe vera is known for its soothing and anti-inflammatory properties. You can either use pure aloe vera gel directly on your gums (be gentle!), or you can rinse with diluted aloe vera juice (mix it with water). The gel's coolness will provide immediate relief, and its anti-inflammatory action will help reduce swelling.
Tea Tree Oil (Use with Caution!)
Tea tree oil boasts powerful antibacterial and antifungal properties. However, it's crucial to dilute it significantly before using it in your mouth. Never apply undiluted tea tree oil directly to your gums. Mix a few drops of tea tree oil with a tablespoon of a carrier oil like coconut or olive oil, then gently dab a small amount onto your gums. Always do a patch test first on a small area of skin to check for any allergic reactions. If you experience any irritation, discontinue use immediately.
Hydrogen Peroxide (Also Use with Caution!)
Similar to tea tree oil, hydrogen peroxide possesses antiseptic qualities that can help fight infection. But again, dilution is essential. Mix a small amount of 3% hydrogen peroxide with an equal amount of water. Swish this solution gently around your mouth for about 30 seconds, then spit it out and rinse thoroughly with plain water. Do not swallow. Use sparingly, as overuse can damage your gums and teeth.
Other Helpful Practices
When to See a Dentist
While these natural remedies can provide relief from mild gum irritation, they aren't a magic bullet. If your symptoms persist or worsen, schedule an appointment with your dentist. This is especially important if you notice:
- Severe pain or swelling
- Persistent bleeding
- Pus formation
- Loose teeth
- Receding gums
Frequently Asked Questions
Q: How long will it take for these natural remedies to work?
A: This varies depending on the severity of your gum infection. You may see improvement within a few days, but for more significant issues, it might take a week or longer. If you don't see improvement after a week, see a dentist.
Q: Can I use these remedies together?
A: Generally, you can use several of these remedies together, but don't overdo it. Start with one or two and see how your gums respond before adding others. Always follow the dilution instructions carefully for hydrogen peroxide and tea tree oil.
Q: Are there any side effects to these natural remedies?
A: While generally safe, some people may experience mild irritation or allergic reactions to certain remedies, particularly tea tree oil and hydrogen peroxide. Always do a patch test before applying anything directly to your gums. If you experience any significant discomfort or adverse reactions, stop using the remedy and consult your dentist or doctor.
Q: Will these remedies cure gum disease?
A: These remedies can help manage the symptoms of mild gum infections, such as gingivitis, but they won't cure advanced gum disease (periodontitis). Advanced gum disease requires professional treatment from a dentist or periodontist.
Q: How can I prevent gum infections in the future?
A: The most important thing is to brush gently and effectively twice a day, floss daily, and maintain a healthy diet. Regular dental checkups and cleanings are also essential for preventing gum disease.
Remember, your oral health is crucial to your overall well-being. Take care of your gums, and they'll take care of you!
Natural Probiotics for Protecting Your Teeth from Decay

Natural Probiotics for Protecting Your Teeth from Decay
Hey everyone! Let's talk teeth. More specifically, let's talk about keeping those pearly whites healthy and decay-free, naturally! We all know brushing and flossing are crucial, but did you know that the power of probiotics can be a game-changer in your oral health routine? It's true! Forget those harsh chemical mouthwashes – let's explore the amazing world of natural probiotics and how they can help protect your teeth from decay.Understanding the Oral Microbiome: It's a Jungle In There!
Your mouth is a bustling city, teeming with millions of bacteria. It's a whole ecosystem, often called the oral microbiome. While some bacteria are beneficial, others, like the Streptococcus mutans gang, are the villains in our tooth decay story. These guys love sugar, and when they feast, they produce acids that attack your tooth enamel, leading to cavities. Yikes!
So, the key is to create a balanced ecosystem where the "good guys" outnumber the "bad guys." And that's where probiotics step in – they're like the superheroes of your mouth!
Introducing Probiotics: The Good Guys of Your Mouth
Probiotics are live microorganisms, mostly bacteria, that offer health benefits when consumed. Think of them as beneficial bacteria that help restore the balance in your gut and, importantly for us today, in your mouth. They work in a few key ways to protect your teeth:
1. Competitive Exclusion: A Bacterial Brawl!
Good probiotic bacteria compete with harmful bacteria for space and resources. It's like a tiny bacterial brawl, and the good guys are winning! By occupying the same spots on your teeth and gums, they prevent the bad bacteria from settling in and causing mischief.
2. Acid Neutralization: The pH Police!
Some probiotics produce substances that neutralize the acids produced by cavity-causing bacteria. Think of them as the pH police, keeping the acid levels in your mouth in check and preventing enamel erosion.
3. Enhanced Immunity: Strengthening Your Defenses!
Probiotics can stimulate your immune system, making it more effective at fighting off infections and inflammation in your mouth. A stronger immune system means less chance of gum disease, which can also contribute to tooth decay.
4. Improved Saliva Composition: A Natural Shield!
Saliva plays a crucial role in protecting your teeth. Some probiotics can help improve the composition of your saliva, making it more effective at neutralizing acids and remineralizing your teeth.
Natural Sources of Oral Probiotics: Where to Find Your Superheroes
You don't need expensive supplements to get your probiotic fix! Many foods naturally contain beneficial bacteria that can promote oral health. Let's explore some delicious options:
1. Yogurt (Especially with Live and Active Cultures):
Look for yogurts that specifically state "live and active cultures" on the label. These cultures contain strains of bacteria like Lactobacillus and Bifidobacteria, known for their beneficial effects on gut and potentially oral health. Try plain yogurt to avoid added sugars.
2. Kefir: The Creamy Probiotic Powerhouse:
Kefir is a fermented milk drink similar to yogurt but with even more diverse probiotic strains. It's tangy, refreshing, and packed with beneficial bacteria.
3. Sauerkraut and Kimchi: Fermented Vegetable Delights:
These fermented vegetables are not only delicious but also contain beneficial bacteria that can contribute to overall gut and potentially oral health. Just remember to rinse your mouth well after consuming them.
4. Kombucha: The Fizz with Benefits:
This fermented tea drink is another great source of probiotics. Choose unsweetened varieties to avoid excess sugar. As with sauerkraut and kimchi, rinsing your mouth afterwards is a good idea.
Beyond Food: Other Ways to Boost Oral Probiotics
While incorporating probiotic-rich foods into your diet is key, there are other ways to support a healthy oral microbiome:
- Maintain good oral hygiene: Brushing and flossing twice a day are still essential for removing food particles and plaque.
- Limit sugary foods and drinks: Sugar feeds the bad bacteria, so reducing your sugar intake is crucial for preventing tooth decay.
- Consider a probiotic mouthwash (consult your dentist): Some probiotic mouthwashes are available, but it's always a good idea to discuss this with your dentist first.
- Manage stress: Stress can impact your immune system, making you more susceptible to oral health problems. Finding healthy ways to manage stress is important for overall health.
Important Considerations
While probiotics offer promising benefits, it's essential to remember that:
- Not all probiotics are created equal: Different strains of probiotics have different effects. More research is needed to determine which strains are most effective for oral health.
- Probiotics are not a replacement for good oral hygiene: They should be seen as a complementary approach, not a substitute for brushing and flossing.
- Consult your dentist or doctor: If you have any concerns or pre-existing health conditions, it's always wise to talk to your healthcare provider before making significant dietary changes.
Commonly Asked Questions
Q: Will probiotics completely prevent tooth decay?
A: While probiotics can significantly improve oral health and reduce the risk of tooth decay, they are not a guaranteed preventative measure. Maintaining good oral hygiene practices remains crucial.
Q: How long does it take to see results?
A: The time it takes to notice improvements in oral health varies from person to person. Consistent intake of probiotics and good oral hygiene are key factors.
Q: Can I take probiotic supplements specifically for oral health?
A: Yes, probiotic supplements specifically formulated for oral health are available. However, it's advisable to consult your dentist or doctor before starting any new supplement regimen.
Q: Are there any side effects associated with consuming probiotics?
A: Side effects are generally rare, but some individuals might experience mild digestive discomfort, such as gas or bloating, particularly when first starting probiotic intake. If you experience any significant side effects, consult your doctor.
I hope this comprehensive guide helps you understand how probiotics can support your oral health journey! Remember, a healthy mouth is a happy mouth – let's work together to keep those smiles shining bright!
The Benefits of Probiotics for Individuals Struggling with Bad Breath

The Benefits of Probiotics for Individuals Struggling with Bad Breath (Halitosis)
Halitosis, commonly known as bad breath, affects a significant portion of the population and can have a detrimental impact on social interactions and self-esteem. While poor oral hygiene is a primary contributing factor, the underlying causes of halitosis are multifaceted and often involve an imbalance in the oral microbiome. Emerging research highlights the potential of probiotics as a complementary therapy to traditional approaches in managing and mitigating bad breath. This article will explore the mechanisms by which probiotics may alleviate halitosis and discuss the evidence supporting their efficacy.
Understanding the Oral Microbiome and its Role in Halitosis
The oral cavity harbors a complex and dynamic ecosystem of microorganisms, collectively known as the oral microbiome. This diverse community comprises bacteria, archaea, fungi, and viruses, which interact with each other and the host in a complex interplay. A healthy oral microbiome maintains a balance, preventing the overgrowth of harmful bacteria responsible for producing volatile sulfur compounds (VSCs). VSCs, primarily hydrogen sulfide, methyl mercaptan, and dimethyl sulfide, are the primary culprits behind the unpleasant odor associated with halitosis.
The Role of Gram-Negative Bacteria
Specific gram-negative anaerobic bacteria, such as Porphyromonas gingivalis, Treponema denticola, and Tannerella forsythia, are strongly implicated in halitosis. These bacteria thrive in anaerobic environments, particularly within periodontal pockets and on the tongue dorsum. Their metabolic processes generate VSCs as byproducts, contributing significantly to bad breath. An imbalance in the oral microbiome, leading to an overgrowth of these VSC-producing bacteria, is a key driver of halitosis.
The Importance of Maintaining Microbial Balance
Maintaining a balanced oral microbiome is crucial for preventing halitosis. A healthy balance involves a diverse community of bacteria, with a lower proportion of VSC-producing species. This balance is achieved through effective oral hygiene practices, such as regular brushing, flossing, and tongue scraping, which remove food particles and bacterial biofilm. However, some individuals may benefit from additional strategies to restore microbial balance, and this is where probiotics come into play.
Probiotics: Restoring Microbial Equilibrium in the Oral Cavity
Probiotics are live microorganisms, primarily bacteria and yeasts, that, when administered in adequate amounts, confer a health benefit to the host. In the context of halitosis, probiotics work through several mechanisms to restore microbial balance and reduce VSC production:
Competition for Resources and Adhesion Sites
Probiotic bacteria compete with pathogenic, VSC-producing bacteria for nutrients and adhesion sites on the tooth surfaces and oral mucosa. By occupying these sites, probiotics effectively limit the growth and colonization of harmful bacteria, preventing their accumulation and VSC production.
Production of Antimicrobial Substances
Certain probiotic strains produce antimicrobial substances, such as bacteriocins and organic acids, that inhibit the growth of other bacteria, including VSC-producing species. These antimicrobial compounds contribute to a reduction in the overall bacterial load and the subsequent decrease in VSC production.
Modulation of the Immune Response
Probiotics can modulate the host's immune response, enhancing the body's ability to combat pathogenic bacteria. They may stimulate the production of antimicrobial peptides and antibodies, further contributing to the control of VSC-producing bacteria and the reduction of halitosis.
Production of Enzymes that Neutralize VSCs
Some probiotic strains produce enzymes that directly neutralize or break down VSCs, reducing their concentration in the oral cavity and subsequently mitigating bad breath. This direct action contributes to a more immediate reduction in halitosis symptoms.
Evidence Supporting the Use of Probiotics for Halitosis
While research on the efficacy of probiotics for halitosis is still ongoing, several studies have demonstrated promising results. These studies have explored various probiotic strains and delivery methods, including chewing gums, lozenges, mouthwashes, and even probiotic-containing toothpastes. The results generally indicate a reduction in VSC levels and an improvement in halitosis scores, although the magnitude of effect varies depending on the specific probiotic strain, the study design, and the duration of intervention.
Challenges and Limitations in Research
It is important to acknowledge certain limitations in the existing research. Studies often have small sample sizes, and the methodologies employed can vary, making direct comparisons challenging. Furthermore, the long-term effects of probiotic interventions on halitosis are not yet fully understood. More large-scale, well-designed clinical trials are needed to definitively establish the efficacy and safety of probiotics for managing halitosis.
Choosing the Right Probiotic for Halitosis
Not all probiotic strains are created equal. Some strains have demonstrated greater efficacy in reducing halitosis than others. Lactobacillus and Streptococcus species have shown particular promise in clinical studies. However, it is crucial to select products that are well-researched and contain strains supported by scientific evidence. Consulting with a dentist or healthcare professional is recommended to determine the most appropriate probiotic strain and dosage for individual needs.
Considerations for Selecting a Probiotic Product
When choosing a probiotic product for halitosis, consider the following factors:
- Strain Specificity: Look for products specifying the exact strain of probiotic bacteria, along with supporting research on its effectiveness for oral health.
- CFU Count: The number of colony-forming units (CFU) indicates the number of live bacteria in the product. Higher CFU counts generally suggest greater efficacy, but this should be considered in conjunction with scientific evidence supporting the specific strain.
- Delivery Method: Probiotics are available in various forms, including chewing gums, lozenges, mouthwashes, and even toothpaste. The optimal delivery method depends on individual preference and compliance.
- Reputable Manufacturer: Choose products from reputable manufacturers who adhere to high quality standards and provide transparent information about their products.
Conclusion
Probiotics offer a promising complementary approach to managing halitosis by restoring microbial balance in the oral cavity. While further research is needed to fully elucidate their efficacy and long-term effects, the available evidence suggests that certain probiotic strains can contribute to a reduction in volatile sulfur compounds and an improvement in breath odor. Incorporating probiotics into an overall oral hygiene strategy, including regular brushing, flossing, and tongue scraping, may provide significant benefits for individuals struggling with bad breath. However, it is essential to consult with a healthcare professional to determine the suitability of probiotic therapy and to select an appropriate product based on individual needs and circumstances.
The Healing Properties of Honey for Gum and Teeth Health

The Healing Properties of Honey for Gum and Teeth Health
For centuries, honey has been recognized not only as a culinary delight but also as a potent natural remedy with diverse therapeutic applications. Its remarkable properties extend to oral health, offering a promising avenue for addressing various gum and teeth issues. This article explores the scientific evidence supporting honey's efficacy in improving oral hygiene and mitigating specific dental problems.
The Composition and Antibacterial Properties of Honey
The multifaceted therapeutic potential of honey stems from its unique composition. Unlike refined sugars, honey boasts a complex blend of natural sugars (fructose and glucose), enzymes, organic acids, vitamins, minerals, and antimicrobial compounds. Crucially, many varieties of honey contain significant levels of hydrogen peroxide, a potent disinfectant. However, the concentration of hydrogen peroxide varies considerably depending on the floral source and processing methods. Furthermore, honey possesses a high osmotic pressure, meaning it draws moisture away from bacteria, hindering their growth and survival.
Antibacterial Mechanisms of Action
Honey's antibacterial efficacy is attributed to several mechanisms:
- Hydrogen Peroxide Production: The enzyme glucose oxidase, present in honey, catalyzes the conversion of glucose to gluconic acid and hydrogen peroxide. This hydrogen peroxide acts as a potent antiseptic, effectively killing or inhibiting the growth of numerous bacteria implicated in oral diseases.
- High Osmotic Pressure: The high sugar concentration in honey creates a hypertonic environment. This draws water out of bacterial cells, leading to dehydration and ultimately cell death. This mechanism is particularly effective against a wide range of microorganisms, including those commonly found in the oral cavity.
- Methylglyoxal (MGO): Certain types of honey, particularly Manuka honey from New Zealand, are rich in methylglyoxal (MGO), a potent antimicrobial compound that contributes significantly to its antibacterial activity. MGO's mechanism of action involves the inhibition of bacterial enzymes and DNA replication, ultimately leading to bacterial cell death.
- Other Antimicrobial Compounds: Beyond hydrogen peroxide and MGO, honey contains a diverse array of other antimicrobial compounds, such as flavonoids, phenolic acids, and other organic compounds. These compounds work synergistically to enhance honey's overall antibacterial effect, providing a broad spectrum of antimicrobial activity.
Honey's Application in Treating Gum Diseases
Gingivitis and periodontitis, collectively known as gum disease, are prevalent oral infections characterized by inflammation and potential destruction of the supporting tissues of the teeth. The bacterial biofilm (plaque) that accumulates on the teeth plays a central role in the pathogenesis of these diseases. Several studies suggest that honey can effectively combat these infections:
Honey's Role in Gingivitis Management
Gingivitis, the early stage of gum disease, is reversible with proper oral hygiene. However, honey can assist in managing the symptoms and preventing progression to more severe forms. Studies have shown that honey-based mouthwashes or topical applications can reduce gingival inflammation, bleeding, and plaque accumulation. The antibacterial and anti-inflammatory properties of honey contribute to these beneficial effects.
Honey in Periodontitis Treatment
Periodontitis, a more advanced stage of gum disease, involves bone loss and potential tooth loss. While honey is not a replacement for conventional periodontal therapy, it may serve as an adjunctive treatment. Research suggests that honey, in conjunction with professional cleaning and scaling, can help reduce the depth of periodontal pockets, improve gingival health, and potentially reduce the need for more invasive procedures. The ability of honey to inhibit the growth of periodontal pathogens, such as Porphyromonas gingivalis, contributes to its therapeutic potential in periodontitis management.
Honey's Potential Benefits for Tooth Health
Beyond its role in gum disease management, honey also displays potential benefits for tooth health:
Cavity Prevention
Dental caries, or cavities, are caused by acid-producing bacteria that metabolize sugars in the oral cavity, leading to demineralization of tooth enamel. While honey contains sugars, its high osmotic pressure and antimicrobial properties may counteract some of these detrimental effects. Some studies suggest that honey may possess a lower cariogenic potential compared to refined sugars, although more research is needed to definitively establish its role in cavity prevention. The antimicrobial properties of honey could help limit the growth of cariogenic bacteria.
Treatment of Oral Ulcers
Aphthous ulcers, or canker sores, are painful oral lesions of unknown etiology. Honey's anti-inflammatory and antimicrobial properties may promote faster healing of these ulcers. Its soothing effect can provide relief from pain and discomfort, speeding up the healing process. The application of honey to canker sores can help to create a protective barrier, preventing further infection and promoting tissue repair.
Limitations and Considerations
While honey offers promising therapeutic benefits for oral health, it's crucial to acknowledge some limitations and considerations:
- Type of Honey: The efficacy of honey can vary significantly depending on the floral source and processing methods. Manuka honey, with its high MGO content, is often cited for its potent antimicrobial properties, but other types of honey can also be beneficial.
- Individual Variation: Responses to honey treatment can vary among individuals. Some people may experience allergic reactions, while others may find its effectiveness limited.
- Not a Substitute for Professional Care: Honey should not be considered a replacement for routine dental checkups and professional dental treatments. It is an adjunctive therapy that complements conventional dental care, not a substitute for it.
- Further Research Needed: While the evidence supporting honey's therapeutic properties is growing, further research is needed to establish its efficacy and safety for various oral health conditions in larger, randomized controlled trials.
Conclusion
The growing body of evidence suggests that honey possesses significant therapeutic potential for improving gum and teeth health. Its inherent antibacterial, anti-inflammatory, and wound-healing properties make it a promising natural remedy for various oral conditions. While honey offers valuable adjunctive therapeutic benefits, it is essential to remember that it should not replace regular dental checkups and professional dental care. Further research is warranted to fully elucidate the scope of honey's efficacy and safety in various oral health applications, paving the way for its wider integration into comprehensive oral healthcare strategies.
Using Probiotics for Healthier Gums and Stronger, More Resilient Teeth

Using Probiotics for Healthier Gums and Stronger, More Resilient Teeth
For centuries, humans have relied on natural remedies to improve their health. Now, scientific research is catching up, revealing the surprising power of probiotics—live microorganisms—in bolstering oral health. Forget the harsh chemicals in many mouthwashes; a growing body of evidence suggests that strategically incorporating probiotics into your routine can lead to healthier gums, stronger teeth, and a significantly improved smile. This article explores the fascinating connection between probiotics and oral health, detailing how these beneficial bacteria contribute to a brighter, healthier future for your teeth and gums.
Understanding the Oral Microbiome and its Impact
Your mouth teems with a complex ecosystem of bacteria, fungi, and viruses—collectively known as the oral microbiome. This microbial community plays a crucial role in maintaining oral health. A balanced microbiome, with a healthy variety of beneficial bacteria, helps prevent the overgrowth of harmful bacteria responsible for gum disease and tooth decay. However, an imbalance, often triggered by poor oral hygiene, a high-sugar diet, or even stress, can lead to a cascade of oral health problems. Harmful bacteria produce acids that erode tooth enamel, leading to cavities, and trigger inflammation in the gums, resulting in gingivitis and periodontitis.
The Role of Probiotics in Oral Health
Probiotics, often referred to as "good bacteria," can help restore balance to the oral microbiome. They achieve this through several mechanisms: They compete with harmful bacteria for resources and space, effectively reducing their numbers. Some probiotics produce substances that inhibit the growth of harmful bacteria, further limiting their impact. Additionally, certain probiotics can strengthen the immune response in the mouth, making it more effective at fighting off infections. This multifaceted approach contributes to a healthier, more resilient oral environment.
Specific Probiotic Strains and their Benefits
Not all probiotics are created equal. Research suggests that specific strains show particular promise in improving oral health. For example, strains like Lactobacillus and Streptococcus have demonstrated effectiveness in reducing gingivitis and plaque formation. These strains exhibit a remarkable ability to colonize the oral cavity, effectively outcompeting harmful bacteria. Further research is ongoing to identify and characterize even more beneficial probiotic strains for optimal oral health outcomes. Always consult with a healthcare professional or dentist before introducing new probiotics into your routine, particularly if you have underlying health conditions.
Incorporating Probiotics into Your Oral Health Routine
There are several ways to incorporate probiotics into your oral health routine. You can find probiotic supplements specifically formulated for oral health, often containing a blend of beneficial strains. These supplements typically come in the form of capsules, tablets, or even lozenges that dissolve in the mouth. Alternatively, you can consume foods naturally rich in probiotics, such as yogurt with live and active cultures, kefir, and sauerkraut. Remember, consistency is key! Regular use of probiotics, alongside good oral hygiene practices (brushing, flossing, and regular dental check-ups), offers the greatest benefits.
Beyond Supplements: A Holistic Approach
While probiotic supplements and probiotic-rich foods are beneficial, remember that maintaining a healthy oral microbiome requires a holistic approach. This includes:
- Practicing meticulous oral hygiene, including brushing and flossing at least twice a day.
- Maintaining a balanced diet low in sugar and processed foods.
- Managing stress levels, as stress can negatively impact the oral microbiome.
- Visiting your dentist regularly for professional cleanings and check-ups.